Executive Summary
Provider Survey on community health worker utilization and impact
Community Health Workers (CHWs) are frontline public health workers who apply a unique understanding of the experience, language, and culture of the population. In 2014, the Centers for Medicaid and Medicare (CMS) issued new guidance that allows for reimbursement of preventive services offered by unlicensed professionals such as CHWs. These developments have tremendous implications for the integration and reimbursement of CHWs in the primary care setting in Arizona. In direct response to monumental shifts in health policy in support of the integration of CHWs in the health care setting, the University of Arizona, Arizona Prevention Research Center (AzPRC) conducted the Community Health Worker Utilization and Impact in the Primary Care Setting Survey. Survey assessed Arizona licensed health care provider perspectives on CHWs impact on patient outcomes, costs and provider time as well as how providers integrate CHWs into primary care the barriers faced to utilization of this workforce. Providers were defined as licensed health professionals, inclusive of physicians, physician assistants, nurse practitioners, psychologists or behavioral health specialists, and pharmacists involved in direct patient care.
The cross-sectional, anonymous, on-line survey was conducted with 364 Arizona providers from various clinical settings including federal qualified community health centers (FQCHC), Indian Health Service and 638 Tribal Clinics and other solo, group, managed behavioral care settings.
Highlights of the survey include:
- 90% of providers reported that CHWs have had a positive impact on patient care.
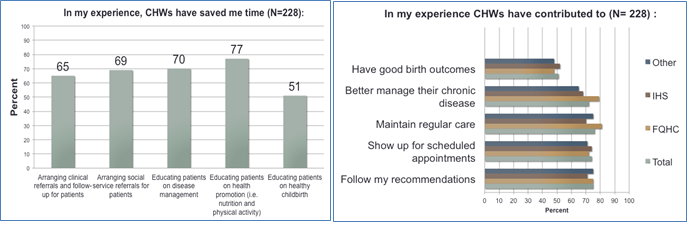
- No less than 70% reported that as a result of working with CHWs their patients were more likely to follow their recommendations, maintain regular care, better mange their chronic disease and have access to care.
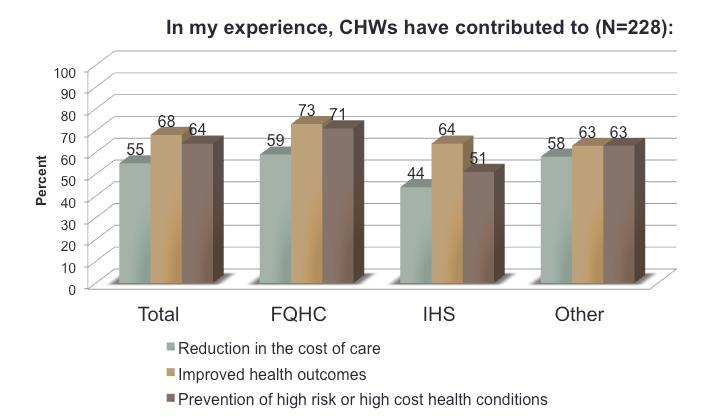
- Approximately 70%, 52% and 63% of FQCHC, IHS/638 and other clinical providers respectively, agree that CHWs have contributed to the prevention of high risk or high cost health conditions

- Half of all providers reported that CHWs saved them time in arranging clinical and social referrals for patients, as well as educating patients on disease management, health promotion and healthy childbirth.
-
Approximately 75% of providers would be more likely to utilize CHWs as part of the health care team if CHWs service were reimbursable by the Center for Medicare and Medicaid Services (CMS) (or AHCCCS in Arizona) or third-party payers.


Summary and Recommendations
- Arizona providers experience great value in the integration of CHWs into the primary care setting to improve health outcomes, reduce cost of care and save provider time.
|
Providers suggested more CHW integration with primary care, including having more CHWs available to meet patient needs in the clinic “Greater integration of CHW services with provider teams including efforts on child health and chronic disease management. More CHWs to provide optimal patient to CHW ratio” -Physician, Indian Health Service/638 “[We need] more CHWs available in clinic to work with a greater percent of patients” Physician, Federally Qualified Community Health Center “A CHW is part of our interdisciplinary team managing a sub-population of high acuity adult patients within our family practice. She is a great asset to the team, and I would like to see CHW services available to our whole population.” Nurse Practitioner, Group Practice
|
The biggest barrier to utilize and integrate CHWs into the health care team is the ability to reimburse and pay for CHW activities. A standardized system that recognizes and reimburses this class of health care worker is required



